At a glance
Rosacea is a chronic skin condition marked by facial redness and discomfort. The cause of rosacea extends beyond the skin, with growing research highlighting the connection between gut health and inflammation. Focusing on digestive wellness and adjusting lifestyle habits can help promote a calmer, more balanced complexion.
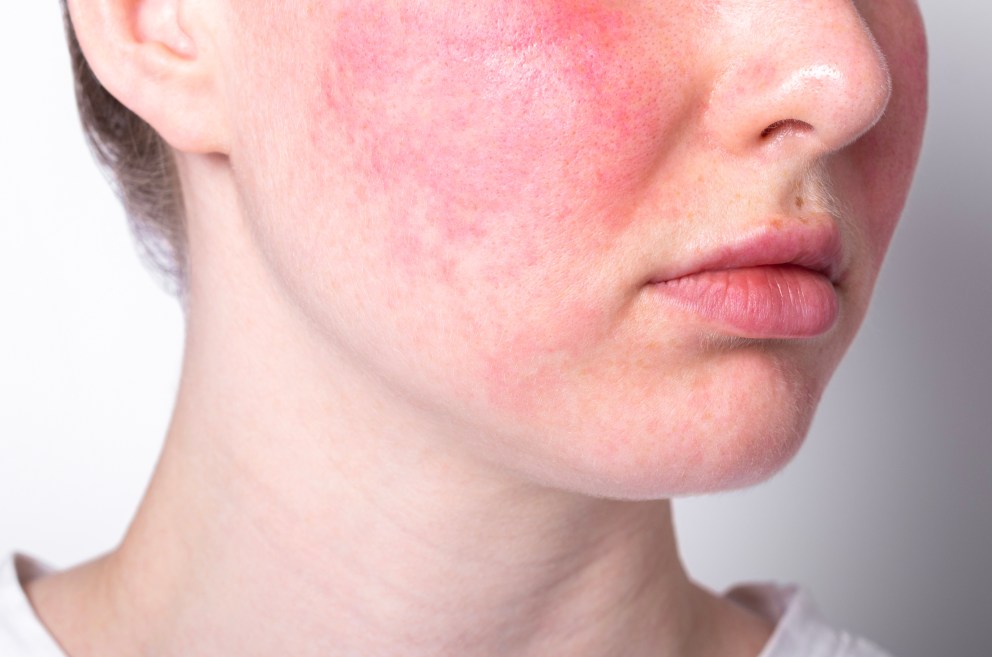
Rosacea is a chronic skin condition that causes persistent redness, burning or stinging sensations, bumps and pimples, and visible blood vessels on the face.
Although the exact cause of rosacea can vary, an imbalanced gut microbiome and overgrowth of potentially harmful microbes in the small intestines have been linked to its development.
Discover the link between microbial imbalances and rosacea and learn about simple but effective diet and lifestyle tips to help manage symptoms naturally.
What is rosacea?
Rosacea is a chronic skin condition that causes facial redness, visible blood vessels, and sometimes swelling or pus-filled pimples. It often affects the cheeks, nose, forehead, and chin.
Although it can occur in anyone, those with darker skin are less likely to develop rosacea than individuals with a lighter skin tone.
Individuals at increased risk of rosacea are those with fair skin between the ages of 30 and 50 or people with a family history of rosacea, acne, or other inflammatory skin conditions.
Rosacea affects women two to three times more than men, and their facial skin symptoms are often more persistent.
Watch the video below to learn about a common, but often overlooked cause, of rosacea.
Signs of rosacea
According to the National Rosacea Society (NRS), there are four main subtypes of rosacea, which affect approximately one in ten adults in the United States.
These include:
- Erythematotelangiectatic rosacea
- Papulopustular rosacea
- Phymatous rosacea
- Ocular rosacea
Symptoms of rosacea commonly fall into several subtypes, and those affected by the condition can experience any combination of symptoms.
1. Erythematotelangiectatic rosacea (ETR)
ETR is the most common form of rosacea, causing skin redness, sensitive skin, enlarged blood vessels, and a burning sensation along the nose, cheeks, and forehead.
2. Papulopustular rosacea
Papulopustular rosacea is associated with the development of papules or pus-filled bumps that resemble acne on the forehead, cheeks, and chin.
3. Phymatous rosacea
Phymatous rosacea is the rarest and most severe subtype that causes facial swelling, skin thickening, and bumps.
Those with phymatous rosacea often experience rhinophyma, which gives the nose a swollen and bulbous appearance.
4. Ocular rosacea
Ocular rosacea causes eye irritation and redness and is typically accompanied by thickened skin, visible small blood vessels, and redness around the nose and cheeks.
Other symptoms of ocular rosacea include light sensitivity and crusty eyelids, as well as dry, rough skin and raised red patches that resemble a rash.
Causes of rosacea
While the exact cause of rosacea isn’t well understood, its development is believed to be attributed to an overactive immune response that leads to chronic skin inflammation.
An imbalance of good and bad gut bacteria, also known as dysbiosis, has also been linked to rosacea, likely because gut microbes play a key role in immune regulation and skin health.
Additionally, an overgrowth of microscopic mites called Demodex folliculorum, which live in hair follicles and oil glands, is strongly associated with skin inflammation and rosacea.
Although these mites are a normal part of the human skin microbiome, an infestation disrupts skin microbiome balance. This can trigger common rosacea symptoms on the face or other parts of the body.

Rosacea triggers
Though they may not be direct causes, several dietary and lifestyle factors are known triggers for rosacea outbreaks in people susceptible to this skin condition.
Sun exposure and extreme hot or cold temperatures may cause rosacea flares by dilating and constricting blood vessels in the face or damaging the skin barrier.
A stressful lifestyle or emotional stress triggers the release of cortisol and adrenaline. These hormones stimulate vasodilation, which impairs skin barrier function and can contribute to rosacea.
Additionally, spicy foods and those that can contribute to gut dysbiosis, such as refined sugars and carbohydrates, can exacerbate facial flushing and the inflammatory response, which can make rosacea symptoms worse.
Alcohol, especially red wine, and hot drinks also stimulate vasodilation and worsen facial skin redness in some individuals.
Other potential triggers include a lack of sleep, use of certain cosmetics and medications, and hormonal imbalances, such as those caused by perimenopause and menopause.
The SIBO and rosacea connection
Small intestinal bacterial overgrowth (SIBO) is characterized by the excessive proliferation of microbes in the small intestine that typically only reside in the large intestine.
While some beneficial microbes are generally present in the small intestine, the overgrowth of certain species, such as Escherichia coli (E. coli), Aeromonas, and Klebsiella, can irritate the gut lining and contribute to intestinal permeability, commonly known as leaky gut.
A compromised gut barrier, especially when SIBO is present, allows bacterial components and by-products to enter the bloodstream. This can trigger systemic immune and inflammatory responses, which are linked to various skin disorders.
Research published in Clinical Gastroenterology and Hepatology concluded, “Rosacea patients have a significantly higher SIBO prevalence than controls. Moreover, eradication of SIBO induced an almost complete regression of their cutaneous lesions.”

Diet and lifestyle tips for rosacea
Rosacea-related skin irritation can significantly impact self-esteem, increasing the risk of anxiety, depression, social isolation, and other physical and emotional effects.
Fortunately, various dietary and lifestyle changes can help support a balanced gut microbiome and reduce the risk of rosacea flare-ups.
Here are six natural tips for rosacea management.
1. Remove sugar and carbohydrates
Refined sugars and carbohydrates promote inflammation, can damage the gut lining if consumed in excess, and act as a primary fuel source for harmful microbes, contributing to SIBO.
Additionally, those with SIBO may notice that their rosacea worsens when consuming vegetables or fermented foods, as fiber and probiotic bacteria can encourage the proliferation of microorganisms in the small intestines.
A short-term carnivore diet helps avoid easily fermentable carbohydrates that exacerbate bacterial overgrowth. This may help heal the intestinal barrier and subsequently improve rosacea.
“The carnivore diet may benefit those with SIBO and leaky gut,” explains Dr. Berg. “Temporarily focusing on animal proteins can promote microbial balance and supply essential amino acids and collagen to support gut repair.”

2. Prioritize antibacterial foods
Clove, oregano, and garlic are rich in natural antibacterial properties, including eugenol, carvacrol, thymol, and allicin. These compounds may help maintain microbial balance within the gut and reduce the proliferation of harmful strains.
A study published in Microbes and Infection found that allicin displayed significant antibacterial activity against various bacteria, including drug-resistant strains of E. coli.
Additionally, apple cider vinegar (ACV) can promote optimal stomach acidity, which helps destroy harmful bacteria before they reach the intestines.
ACV may also support healthy digestion by improving stomach acid levels, which helps break down food properly and reduces the chance of undigested food feeding microbes in the intestines.
3. Practice prolonged fasting
Prolonged fasting may induce xenophagy, a selective form of autophagy in which the body degrades harmful microbes, such as bacteria, fungi, and viruses, that could compromise health.
By directly targeting bacterial overgrowth, xenophagy supports the natural balance of microorganisms in the gut and mitigates symptoms of SIBO-related rosacea.
Additionally, fasting-induced autophagy has been shown to regulate key inflammatory pathways, potentially lowering an overactive response to stimuli that can trigger rosacea flares.

4. Protect your skin from the elements
Protecting your skin from the sun, cold weather, and harsh wind can help protect the delicate skin barrier from extreme temperatures that can aggravate symptoms of rosacea.
Applying natural sunscreen and wearing a hat, long-sleeved shirts, pants, scarves, and other protective clothing can minimize exposure to the elements and reduce the risk of flare-ups from environmental stressors.
5. Manage stress
Managing chronic stress helps lower cortisol levels and calms an overactive immune system, which may otherwise worsen rosacea symptoms.
Breathing techniques, exercise, long walks, mindfulness, and engaging in hobbies are great ways to ease tension and relax the body.

When to talk to your doctor
If left untreated, severe cases of rosacea can lead to facial disfigurement and significant psychophysical consequences.
Those experiencing rosacea symptoms should consult their healthcare provider to discuss treatment options.
Initial treatment for rosacea typically involves topical medications and a gentle skin care routine to minimize irritation and restore skin microbiome balance.
Depending on the underlying cause, oral treatments, such as antibiotics and anti-inflammatory drugs, can also be considered. These medications aim to treat and prevent rosacea from worsening by eliminating pathogenic skin mites and downregulating immune responses.
Most symptoms improve with topical treatments or medication. However, in severe cases, rosacea patients may be prescribed laser procedures to remove visible blood vessels and improve skin appearance.
Key takeaways
- Rosacea is a chronic skin condition that causes facial redness, visible blood vessels, and occasional irritation.
- Common triggers include stress, alcohol, spicy foods, and temperature extremes, which can inflame sensitive skin.
- While the cause of rosacea can differ between individuals, microbial imbalances in the gut and excess inflammation may play a role.
- Supporting gut and inflammatory balance with a nutrient-rich diet, good hydration, and minimal refined sugars may promote clearer skin.
- Managing stress, getting enough rest, and protecting the skin from harsh environments can help maintain long-term skin resilience.
FAQ
1. What is the root cause of rosacea?
2. What is the biggest trigger for rosacea?
3. How can I clear up my rosacea?
4. Is rosacea caused by a virus or bacteria?
5. How is rosacea treated?
Sources
- “Classification of Rosacea.” National Rosacea Society. Classification of Rosacea | Rosacea.org. rosacea.org.
- Parodi A, Paolino S, Greco A, et al. Small intestinal bacterial overgrowth in rosacea: clinical effectiveness of its eradication. Clin Gastroenterol Hepatol. 2008;6(7):759-64. doi:10.1016/j.cgh.2008.02.054
- Ankri S, Mirelman D. Antimicrobial properties of allicin from garlic. Microbes Infect. 1999;1(2):125-9. doi:10.1016/s1286-4579(99)80003-3