At a glance
A distended belly can be caused by either excess abdominal fat or fluid buildup, also known as ascites. While belly fat develops and is linked to lifestyle and diet habits, ascites is often indicative of liver disease and can appear rapidly. Recognizing the differences between ascites and belly fat is essential for appropriate management and medical care.
A large and distended belly isn’t always caused by excessive fat deposits.
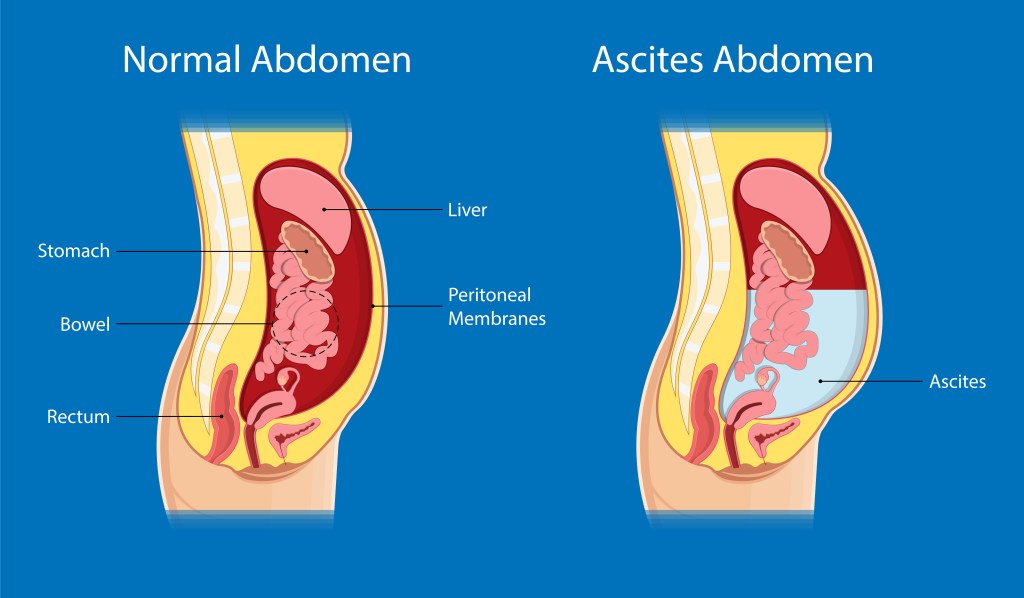
Ascites is the accumulation of excess fluid in the abdominal cavity, and belly fat is caused by visceral and subcutaneous fat around abdominal organs and the abdominal wall.
While both conditions lead to extended waistlines and weight gain, the causes and management of excess abdominal fluid and visceral belly fat are distinctly different.
Let’s look at the difference between ascites and belly fat and how to minimize fluid in the abdomen.
Ascites vs. belly fat
Ascites and belly fat are two different conditions that cause an enlarged and distended abdomen and increased body weight.
Ascites can indicate serious liver disease, and it’s important to know how to spot the difference between abdominal fat and fluid accumulation.
What is ascites?
Ascites is a medical condition that typically develops due to liver disease and is characterized by excessive fluid accumulation in the peritoneal cavity, which is the space surrounding digestive organs and the liver.
Chronic alcohol intake, liver infections, and hepatitis can cause cirrhosis and scarring of liver tissue. Because liver cells filter blood, liver scarring can lead to elevated blood pressure in abdominal blood vessels, which causes fluid to leak from the portal vein, the liver’s main blood supply, into the abdominal cavity.
When fluid leaks from blood vessels, blood volume drops and signals a state of dehydration to the kidneys, causing water retention and more fluid accumulations, which worsens ascites.
What is belly fat?
Belly fat develops due to excessive fat deposits of two different types of fats within the abdomen.
Visceral fat is linked to central obesity and accumulates around organs. Subcutaneous fat is the layer of fat between your skin and the abdominal wall.
While subcutaneous fat typically isn’t a cause for serious health concerns, research published in the Journal of Lipids in Health and Disease suggests that visceral fat increases the risk of heart disease, diabetes, and cancer.1
Risk factors linked to excess body fat mass and belly fat include:
- Poor diet
- Excess calorie intake
- Sedentary lifestyle
- “The Liver Body Type–Explanation and Symptoms | Dr. Berg.” Dr. Berg. https://www.drberg.com/blog/the-liver-body-type
- Stress
- Lack of sleep
It’s important to understand that an enlarged abdomen can indicate potentially serious health problems.
If you have developed a swollen abdomen or experience rapid, unexplained weight gain, consult with a healthcare provider to determine all possible underlying causes and formulate an appropriate treatment plan based on your individual symptoms and health status.
Watch the video below to learn what steps you can take to ease symptoms of ascites.
How do you know if you have ascites or belly fat?
Ascites typically develops over a few weeks or months and is characterized by a significant change in body shape and a smooth belly that feels hard to the touch.
Common symptoms of ascites include frequent urination, difficulty breathing, swollen feet and legs, hemorrhoids, and nausea.
In contrast to ascites, belly fat causes a soft belly that tends to develop slowly due to poor dietary and lifestyle habits.
While belly fat doesn’t cause significant symptoms, excess fat around the organs can impact cardiovascular functioning and cause shortness of breath and hypertension.
Causes of ascites
Ascites is a serious medical condition that indicates impaired kidney and liver function and may require immediate treatment.
Factors that can cause or contribute to ascites include:
- Hepatitis B or C infections
- Chronic alcohol abuse
- Fatty liver disease
- Genetic predisposition to cirrhosis
- Congestive heart failure
- Ovarian cancer
- Portal hypertension
How to get rid of ascites
Depending on the severity of abdominal fluid, conventional ascites treatment includes diuretic medications to stimulate fluid loss, drainage of excess abdominal fluid, and modifications of sodium intake. In some extreme cases, the loss of liver function may require a liver transplant.
Fortunately, you can take several steps to lower your risk of ascites and support healthy kidney and liver function.
1. Practice intermittent fasting
Intermittent fasting is a pattern of meal time scheduling that includes prolonged periods without calorie intake.
A study published in Aging Research Reviews suggests that fasting has profound beneficial metabolic effects and triggers autophagy, a biochemical process that degrades old, damaged cells and stimulates cellular renewal.2
According to Dr. Berg, “Intermittent fasting has been shown to enhance liver cell function and can help improve liver function, which is crucial in managing ascites.”
2. Incorporate antioxidant-rich foods
The liver is the body’s main metabolic and detoxification organ, which significantly increases the rate of oxidative stress within liver cells.
Energy production, alcohol detoxification, and the breakdown of hormones, drugs, and environmental toxins create free radicals, highly volatile chemical compounds linked to liver cell damage and inflammation.
Antioxidants are naturally occurring compounds that have been shown to neutralize free radicals in liver cells and protect liver tissue from scarring.
Some of the best antioxidant-rich foods include:
- Berries
- Cruciferous vegetables
- Green leafy vegetables
- Dark chocolate
- Seeds and nuts
- “Health Benefits of Green Tea Explained Clearly | Dr. Berg.” Dr. Berg. https://www.drberg.com/blog/the-amazing-health-benefits-of-green-tea
- Garlic
- Turmeric
3. Follow a low-carb diet
A nutrient-dense, low-carb approach like Healthy Keto® may help support liver health by aligning with the body’s natural mechanisms that manage oxidative balance within liver cells.
In contrast, high carbohydrate intake can lead to rapid energy production, which may elevate free radical formation and potentially contribute to oxidative stress and inflammation in the liver.
4. Avoid alcohol
Alcohol, or ethanol, is cytotoxic, meaning it directly impacts cellular health and causes damage to cell structures and DNA.
Liver cells detoxify alcohol, making the liver especially susceptible to alcohol-related damage and cirrhosis.
According to a study published in the Journal of Alcohol Research, “Heavy ethanol consumption produces a wide spectrum of hepatic lesions, the most characteristic being fatty liver (i.e., steatosis), hepatitis, and fibrosis/cirrhosis.”3
Key takeaways
- Belly fat is generally caused by excessive calorie intake, high-carb diets, and a sedentary lifestyle.
- Ascites is characterized by the accumulation of excess fluid in the abdominal cavity and is typically associated with liver dysfunction.
- Compared to belly fat, ascites develops quickly and often causes a firm, smooth, and tight abdomen.
- Combining intermittent fasting with a low-carb, nutrient-dense diet and antioxidant-rich foods helps support liver health and may reduce fluid accumulation.
- Ascites requires a thorough medical evaluation to determine the underlying causes and formulate an appropriate treatment plan.
FAQ
What does an ascites belly feel like?
How do you rule out ascites?
How can I check if I have ascites at home?
What is the difference between a beer belly and ascites?
How does ascites feel to the touch?
How do I know if I have fat or fluid in my abdomen?
Do you gain weight with ascites or belly fat
Is ascites fluid?
Sources
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6138918/ ↩︎
- https://pubmed.ncbi.nlm.nih.gov/30172870/ ↩︎
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5513682/ ↩︎


















