At a glance
Blood sugar levels measure the amount of glucose circulating in the bloodstream. This glucose fuels cells for energy, while excess amounts are stored for later use. Maintaining balanced blood sugar levels is important, as ongoing imbalances can interfere with normal body function and are linked to broader metabolic health concerns, including heart disease, kidney problems, and diabetes.
Maintaining steady blood sugar levels is crucial for metabolic health, hormonal balance, and effective weight management. But what is a normal blood sugar level?
Discover what is considered a healthy blood sugar range, why blood glucose testing is essential, and how to support glucose balance.
What are blood sugar levels?
Blood sugar levels, also called blood glucose levels, refer to the amount of glucose circulating in the bloodstream at the time of testing.
Glucose is the body’s primary fuel source and is obtained from the foods you consume, primarily from sugars and carbohydrate-rich foods.
If available, your cells utilize blood sugar for immediate energy use. If blood sugar levels exceed the body’s energy needs, surplus glucose is stored in the liver and muscles as glycogen or converted into fat for later use.
This explains why consistently elevated blood sugar levels, typically linked to a high-carb diet, are a primary cause of weight gain, obesity, and metabolic imbalances.
While chronically high blood sugar levels are linked to poor health outcomes, frequent low blood sugar levels can also be detrimental and may be indicative of serious underlying medical issues.
Watch the video below to learn how to maintain normal blood sugar levels.
Why your blood sugar levels matter
Blood sugar levels are a key marker of overall health, and an impaired fasting glucose measurement may indicate that the body struggles to maintain blood sugar balance.
While glucose provides cellular energy, persistently elevated blood sugar levels can damage blood vessels and organs, increasing the likelihood of heart disease, kidney problems, and other serious health problems.
In addition, poor blood sugar control is a significant diabetes risk factor, and early detection of elevated glucose concentrations is vital to reduce the risk of health problems.
Research published in StatPearls underscores the importance of regular glucose monitoring for both hyperglycemia and hypoglycemia, summarizing, “Very high or very low blood glucose levels could impair cellular function and may be lethal if not managed appropriately.”
Hyperglycemia refers to elevated blood sugar, while hypoglycemia describes abnormally low levels. Both conditions disrupt the body’s ability to maintain stable energy and can lead to serious health complications.
The American Diabetes Association (ADA) released a report recommending that all individuals over 35 years of age, pregnant women, and younger people who are overweight, obese, or have risk factors for diabetes, undergo regular blood glucose testing.
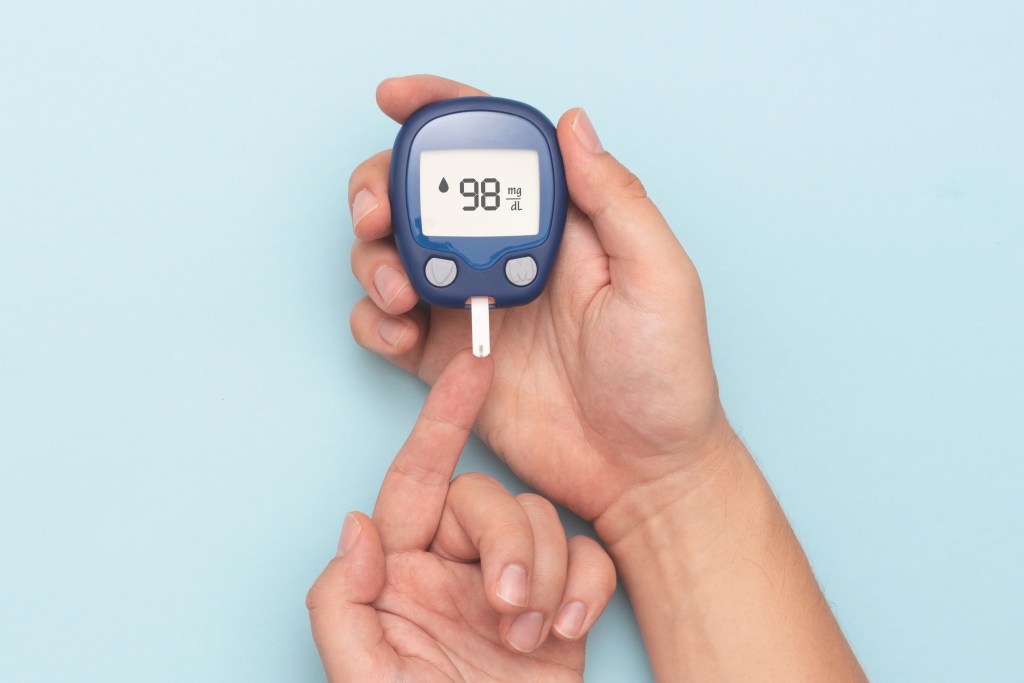
Testing your blood sugar levels
Blood sugar levels can be checked at home with a glucose meter that uses a finger prick and test strip, or through a healthcare provider who measures fasting plasma glucose with a blood sample.
While at-home tests provide a convenient way to track daily blood sugar changes, they don’t assess long-term glucose control, which is determined by measuring glycated hemoglobin A1C (HbA1C).
When blood contains excessive amounts of blood sugar, glucose molecules start to attach to hemoglobin proteins, creating HbA1C.
HbA1C testing requires a laboratory blood test and indicates the average blood sugar levels over the past three months. This marker is widely used to identify metabolic health issues and assess the risk of diabetes mellitus, also known as type 2 diabetes.
Some individuals, especially those with type 1 diabetes, can benefit from using a continuous glucose monitor. This device, which is placed on the skin, continuously tracks glucose levels and transmits real-time readings to a monitor or smartphone.
What is a normal blood sugar level?
Blood sugar levels can fluctuate significantly during the day due to food intake, physical activity, and other factors that influence how the body processes and regulates glucose.
For this reason, it’s recommended to measure glucose in a fasted state to obtain a consistent baseline.
Normal glucose levels for adults in a fasted state range between 70 to 99 mg/dl, which is equivalent to 3.9 to 5.6 mmol/L.
Blood sugar levels measured postprandial, meaning two hours after a meal, shouldn’t exceed 140 mg/dL, or 7.8 mmol/L, to remain in a normal range.
Normal fasting blood sugar test results for children and teens are similar to those of adults, ranging from 70 to 99 mg/dL.
Postprandial levels for younger age groups should also remain under 140 mg/dL (7.8 mmol/L), although slightly higher readings may occasionally occur depending on physical activity and growth stage.
HbA1C levels of less than 5.7 percent are considered normal for adults, teens, and children and signal healthy long-term blood sugar control with a low risk of diabetes-related complications.
What does a high blood sugar level mean?
Elevated blood sugar levels after a meal are common and typically linked to eating sugary foods or carbohydrate-rich meals.
However, postprandial levels greater than 140 mg/dL or fasting glucose concentrations above 99mg/dL indicate poor blood sugar regulation and insulin resistance.
A diet high in refined carbohydrates and sugars causes persistent blood sugar elevations, which trigger continuous insulin release to maintain balance.
Over time, this constant insulin signaling can reduce cellular responsiveness to insulin, making it harder for glucose to enter cells. Insulin resistance worsens blood sugar control and contributes to the development of diabetes.
Fasting blood sugar levels exceeding 100 mg/dL (5.7 mmol/L) are classified as pre-diabetic, and results greater than 126 mg/dL (7.0 mmol/L) indicate diabetes.
To support optimal glucose control and mitigate the risk of diabetes, it’s essential to maintain a healthy weight, follow a nutritious diet, and check your blood sugar levels regularly.
Research published in Diabetes Care reports that a low-carb ketogenic diet promotes blood sugar balance and can significantly improve hyperglycemia, thereby reducing the risk of diabetes and associated health issues.
Other steps to help lower blood sugar levels include:
- Avoid processed foods
- Engage in regular physical activity
- Prioritize sleep and stress management
- Maintain a healthy body weight
- Avoid excessive amounts of lean protein

What does a low blood sugar level mean?
A fasting blood glucose test result below 70 mg/dL (3.9 mmol/L) is a sign of low blood sugar, often caused by skipping meals, vigorous exercise, drinking alcohol on an empty stomach, or stressful events.
However, hypoglycemia can also be triggered by poorly controlled type 1 diabetes or taking too much insulin or other diabetes medicines that cause a sudden drop in blood sugar levels.
Low glucose levels can typically be managed by consuming a meal to help regulate blood sugar levels and prevent fluctuations.
Supporting metabolic health through a nutrient-dense diet, such as a well-formulated low-carb Healthy Keto® plan, can also help maintain long-term blood sugar balance.
While it may seem counterintuitive, limiting carbohydrate and sugar intake can help prevent hypoglycemia by minimizing blood sugar spikes and crashes, keeping glucose levels more stable.
However, severe cases of hypoglycemia, characterized by blood glucose levels below 54 mg/dL (3.0 mmol/L), require prompt medical care to prevent serious complications.

The dawn phenomenon
The dawn phenomenon is a natural rise in blood sugar that occurs in the early morning, usually between 2:00 to 8:00 a.m.
It happens when the body releases hormones linked to the circadian rhythm, such as cortisol, which signal the liver to release stored glucose to provide energy for waking and starting the day.
“In healthy individuals, the body can regulate rising blood sugar levels by releasing insulin”, explains Dr. Berg. “However, those with insulin resistance, pre-diabetes, or diabetes may not produce enough insulin to balance glucose, resulting in higher-than-normal morning blood sugar levels.”
Understanding the dawn phenomenon is crucial to correctly evaluating blood sugar readings, especially those taken at home, as it can impact fasting measurements and overall diabetes management strategies.

When to talk to your doctor
Both hypo- and hyperglycemia can have serious health consequences, so it’s vital to consult a healthcare provider if you are concerned about your blood glucose levels.
Symptoms of poor blood sugar control may include unexplained weight changes, fluid retention and swelling, excessive thirst, frequent urination, blurred vision, fatigue, and slow-healing wounds.
Recognizing these signs early and seeking medical guidance can help prevent long-term complications such as diabetes, heart disease, kidney damage, nerve problems, and vision loss.
A doctor will evaluate your symptoms and risk factors and may recommend tests to evaluate your metabolic health and formulate a treatment strategy to achieve and maintain healthy blood sugar targets.
If you track blood sugar levels as part of your diabetes care plan and notice readings consistently above or below your target range, it’s important to contact your healthcare provider promptly.
In addition, it’s vital to consult a doctor immediately if you show signs of severe hypoglycemia, such as confusion, seizures, loss of consciousness, or an inability to eat or drink.
This is a medical emergency and requires prompt treatment to prevent serious complications or life-threatening outcomes.
Key takeaways
- Understanding what is a normal blood sugar level, is important for maintaining overall metabolic health.
- Normal fasting blood sugar levels range from 70 to 99 mg/dL, and postprandial levels should not exceed 140 mg/dL.
- Blood sugar levels consistently above these ranges can indicate diabetes, while levels below 70 mg/dL suggest hypoglycemia, both of which require monitoring and medical attention.
FAQ
1. What is a normal blood sugar level for adults?
2. What are the signs that your blood sugar is too high?
3. What is a prediabetic blood sugar level?
4. When would I need a blood glucose test?
5. What is a good blood sugar level in the morning?
Sources
- Kesson CM, Lawson P, Ireland JT. Monitoring blood glucose. Br Med J. 1980;280(6209):253.3-253. https://www.ncbi.nlm.nih.gov/books/NBK555976/
- https://diabetesjournals.org/care/article/48/Supplement_1/S27/157566/2-Diagnosis-and-Classification-of-Diabetes
- Davis NJ, Tomuta N, Schechter C, et al. Comparative study of the effects of a 1-year dietary intervention of a low-carbohydrate diet versus a low-fat diet on weight and glycemic control in type 2 diabetes. Diabetes Care. 2009;32(7):1147-52. https://pubmed.ncbi.nlm.nih.gov/19366978/


















