At a glance
Polycystic ovarian syndrome (PCOS) is a hormonal condition characterized by immature ovarian follicles that can disrupt ovulation, menstrual cycles, and fertility. The condition is closely linked to hormonal imbalances and insulin resistance, which can influence weight, skin health, and reproductive function. Because PCOS can also affect long-term metabolic health, recognizing its causes and symptoms helps support early evaluation and management.
Polycystic ovarian syndrome or polycystic ovary syndrome (PCOS) is a relatively common hormonal disorder affecting women of reproductive age.
PCOS is closely linked to metabolic health and dietary habits, and women who consume excessive amounts of sugar and refined carbohydrates are at higher risk of developing ovarian cysts.
Discover the underlying cause of PCOS and learn how making simple dietary and lifestyle changes can support hormonal balance and promote female health and well-being.
What is polycystic ovarian syndrome?
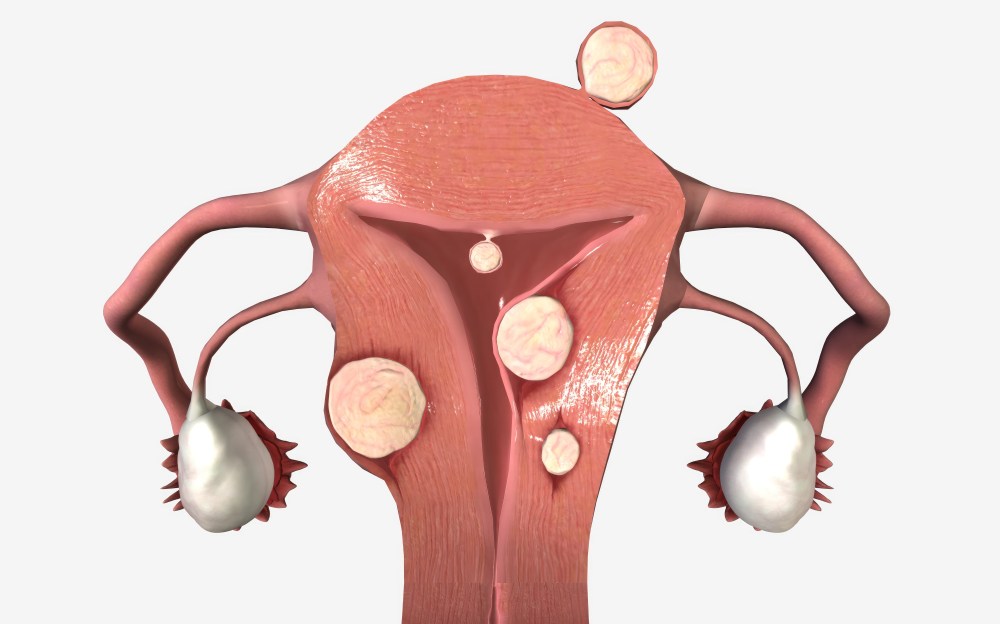
Polycystic ovarian syndrome (PCOS) is characterized by the development of ovarian cysts, which are fluid-filled sacs that form on the ovaries when eggs don’t mature properly during the menstrual cycle.
Polycystic ovaries can contain several immature follicles, which can cause ovarian enlargement, hormonal imbalances, menstrual irregularities, body weight changes, and infertility.
The National Institute of Child Health and Human Development (NICHD) released data indicating that PCOS is a common cause of infertility, noting that many women are unaware they have PCOS until trying to conceive.
PCOS is typically present when at least two diagnostic criteria are met. These include irregular or absent ovulation, elevated androgen levels, or clinical signs such as excess body or facial hair, and polycystic ovaries containing clusters of immature follicles.
Research published in the Journal of Reproductive Science suggests that as many as 20 percent of women develop PCOS, with dietary and lifestyle factors suggested as key contributors.
Watch the video below to discover the common, but often overlooked, cause of PCOS.
Symptoms of polycystic ovarian syndrome
Polycystic ovaries typically don’t cause pain or discomfort, and many women with PCOS are unaware they have the condition until they experience health problems related to the hormone imbalances underlying its development.
Common PCOS symptoms include:
- Irregular menstrual cycle
- Infertility
- Oily or acne-prone skin
- Unexplained weight gain
- Excess hair growth, especially facial hair
- Male pattern hair thinning or hair loss
- Mood changes
In addition, women with PCOS tend to be at an increased risk of other health conditions, such as
high blood pressure, metabolic syndrome, heart disease, endometrial cancer, and diabetes.
This highlights the importance of seeking medical support for early PCOS diagnosis, as well as regular monitoring and effective treatment strategies to minimize long-term health risks.

Causes of polycystic ovarian syndrome
While genetic predisposition and a family history can increase the risk of this PCOS, evidence published in Cureus confirms the direct link between insulin resistance and the development of polycystic ovaries.
Insulin is a key metabolic hormone involved in blood sugar control. Insulin resistance develops when cells become less responsive to insulin signaling, causing insulin levels and blood sugar to rise.
High insulin levels affect hormone production in the ovaries, disrupting the balance between follicle-stimulating hormone (FSH) and luteinizing hormone (LH). This imbalance often leads to the growth of multiple immature follicles, resulting in polycystic ovaries.
In addition, elevated insulin levels stimulate the ovaries to produce more androgens, including testosterone.
Higher androgen levels further disrupt hormonal balance, contribute to irregular shedding of the uterine lining, promote excess body hair growth, affect weight management, and influence other aspects of female health.
Insulin resistance is strongly linked to a diet high in refined carbohydrates, sugars, and ultra-processed foods (UPFs).
These foods trigger frequent spikes in insulin, and over time, the body’s cells become less responsive, creating a vicious cycle of increasing insulin levels and worsening hormonal imbalance.
Research published in Aspects of Molecular Medicine summarizes, “Chronic consumption of high-sugar UPFs contributes substantially to total dietary sugar intake, creating a metabolic environment conducive to the development of insulin resistance.”

Healthy lifestyle tips for PCOS
Because PCOS development is linked to a poor diet, making beneficial dietary and lifestyle changes is a simple but effective strategy to manage PCOS.
Here are six healthy lifestyle tips for PCOS.
1. Follow a low-carb diet
A study published in the Journal of the Endocrine Society found that PCOS women who followed a low-carb ketogenic diet plan for six weeks showed markedly reduced androgen levels and overall improved hormonal markers.
Restricting carbohydrate intake to no more than 50 grams per day supports insulin sensitivity and can help reverse insulin resistance, making keto an effective dietary approach for PCOS management.
A whole-food-based and nutrient-focused low-carb diet, such as Healthy Keto®, not only limits carbohydrates and sugars but also avoids processed foods, which have been linked to worsening insulin resistance and consequently PCOS.
In addition, following a low-carb diet supports weight loss and promotes metabolic balance, two crucial aspects of restoring hormonal balance and managing PCOS-related symptoms.

2. Practice intermittent fasting
Intermittent fasting is a mealtime schedule that alternates between periods of caloric restriction and time-set eating windows.
A 16:8 fast is a popular intermittent fasting approach that involves fasting for 16 hours, followed by an 8-hour period during which two meals are consumed.
“Limiting meal frequency reduces the body’s need for insulin,” explains Dr. Berg. “This allows your cells to reset and increases their responsiveness to insulin, which helps prevent and manage insulin sensitivity.”
Evidence published in the Journal of Translational Medicine supports this, highlighting that a time-restricted mealtime schedule significantly improved insulin sensitivity, inflammatory markers, and menstrual regularity in women with PCOS.
3. Maintain a healthy body weight
Being overweight increases the risk of both insulin resistance and PCOS. It’s believed that excess fat tissue interferes with insulin function and disrupts normal hormone production, which can worsen androgen imbalances and contribute to polycystic ovaries.
Combining Healthy Keto with intermittent fasting, regular exercise, and focusing on optimal sleep quality is an excellent strategy for achieving and maintaining a healthy body weight.

4. Incorporate effective stress management
Chronic stress is detrimental to overall health and well-being and can worsen PCOS symptoms.
Elevated levels of the stress hormone cortisol can interfere with insulin balance and insulin signalling and have been linked to increased testosterone release.
This explains why stress can contribute to hormonal imbalances, contributing to symptoms such as excess body hair, acne, irregular menstrual cycles, and challenges with weight management.
Relaxation techniques such as deep breathing, connecting with loved ones, engaging in hobbies, or spending time in nature can help reduce daily stress and support hormone balance.
5. Support liver function
Promoting optimal liver function is critical for maintaining the body’s hormonal balance, a key factor for managing PCOS.
The liver plays a central role in the metabolism and detoxification of hormones. If the liver isn’t functioning well, hormones can accumulate, contributing to elevated testosterone linked to PCOS.
Minimizing the intake of processed foods while prioritizing leafy greens, cruciferous vegetables, healthy fats, and high-quality protein can help support liver function and promote efficient hormone metabolism.

6. Minimize exposure to endocrine disruptors
Evidence published in Life found that PCOS severity may be linked to excessive exposure to bisphenol A (BPA), an endocrine disruptor that can contribute to hormonal imbalances.
The study found that women with PCOS appear to have higher urinary concentrations of BPA, which appears to modulate enzymatic activity within hormone-producing cells in the ovaries.
BPA is a widely used chemical found in numerous plastic products, including food storage containers, plastic tableware, and water bottles.
Therefore, it’s recommended to carefully check products for BPA content and opt for glass, stainless steel, or BPA-free alternatives whenever possible.
Reducing exposure to BPA and other endocrine-disrupting chemicals can help support hormonal balance, improve ovarian function, and potentially lessen the severity of PCOS symptoms.

When to talk to your doctor
It’s important to consult a healthcare provider if you are concerned about PCOS, have developed irregular periods, or are experiencing other symptoms associated with polycystic ovaries, including unusual hair growth, acne, weight gain, or mood changes.
A medical professional can assist in diagnosing PCOS by evaluating symptoms, discussing your medical history, and performing blood tests and imaging studies.
Conventional PCOS treatment typically involves a combination of lifestyle changes and medications, including oral contraceptives and drugs to improve insulin sensitivity.
It’s also vital to seek medical care if you have difficulties conceiving. Reproductive medicines, fertility treatments, or in vitro fertilization (IVF) can help women with PCOS achieve a successful pregnancy.
Key takeaways
- Polycystic ovarian syndrome (PCOS) is a common hormonal condition that can influence menstrual cycles, fertility, and long-term metabolic health.
- Supporting insulin sensitivity and maintaining a healthy weight play an important role in managing PCOS symptoms.
- A nutrient-focused low-carb diet combined with intermittent fasting may help promote better hormonal balance and metabolic function.
FAQ
1. What is polycystic ovarian syndrome?
2. What complications are associated with PCOS?
3. What should you avoid if you have PCOS?
4. Can I still get pregnant if I have PCOS?
Sources
- Deswal R, Narwal V, Dang A, Pundir CS. The Prevalence of Polycystic Ovary Syndrome: A Brief Systematic Review. J Hum Reprod Sci. 2020;13(4):261-271. https://pmc.ncbi.nlm.nih.gov/articles/PMC7879843/
- Purwar A, Nagpure S. Insulin Resistance in Polycystic Ovarian Syndrome. Cureus. 2022;14(10):e30351. https://pmc.ncbi.nlm.nih.gov/articles/PMC9665922/
- Babalola OO, Akinnusi E, Ottu PO, et al. The impact of ultra-processed foods on cardiovascular diseases and cancer: Epidemiological and mechanistic insights. Aspects of Molecular Medicine. 2025;5:100072. https://www.sciencedirect.com/science/article/pii/S2949688825000103
- Khalid K, Apparow S, Mushaddik IL, Anuar A, Rizvi SAA, Habib A. Effects of Ketogenic Diet on Reproductive Hormones in Women With Polycystic Ovary Syndrome. J Endocr Soc. 2023;7(10):bvad112. https://pmc.ncbi.nlm.nih.gov/articles/PMC10484165/
- Li C, Xing C, Zhang J, Zhao H, Shi W, He B. Eight-hour time-restricted feeding improves endocrine and metabolic profiles in women with anovulatory polycystic ovary syndrome. J Transl Med. 2021;19(1):148. doi:10.1186/s12967-021-02817-2 https://pubmed.ncbi.nlm.nih.gov/33849562/
- Tinkara Srnovršnik, Irma Virant-Klun, Bojana Pinter. Polycystic Ovary Syndrome and Endocrine Disruptors (Bisphenols, Parabens, and Triclosan)—A Systematic Review. Life. 2023;13(1):138. doi:10.3390/life13010138 https://pmc.ncbi.nlm.nih.gov/articles/PMC9864804/