At a glance
The thyroid is a small gland located at the base of the neck that produces hormones essential for metabolism, energy production, and body temperature regulation. Its function depends on proper hormone signaling between the thyroid and pituitary glands. Balanced thyroid health supports nearly every system in the body, yet millions experience undiagnosed thyroid disorders that can impact long-term well-being.
The thyroid gland makes and releases thyroid hormones, which regulate many of your body’s vital processes, including energy production, body temperature, and heart rate.
Imbalanced thyroid levels can result from various thyroid problems and may increase the risk of fatigue, mood changes, heart issues, weight gain, and many other health complications.
Let’s look at five common thyroid disorders and learn how beneficial dietary and lifestyle changes can support thyroid gland function and hormonal balance.
What is the thyroid?
The thyroid is a small, butterfly-shaped gland located at the base of the neck. It’s an essential part of the body’s endocrine system, which controls critical physiological functions through hormone signalling.
The thyroid gland produces thyroid hormones, primarily T4 (thyroxine) and T3 (triiodothyronine). T4 is considered the inactive form, which the body converts into active T3 to regulate metabolic pathways, body temperature, energy utilization, and various cellular functions.
The production of thyroid hormone is controlled by the pituitary gland, a small gland in the brain that releases thyroid-stimulating hormone (TSH).
When thyroid hormone levels are too low, the pituitary increases TSH to signal the thyroid gland to produce more. When thyroid hormone levels are too high, TSH is reduced to slow production.
A healthy thyroid and balanced hormone levels are essential for overall well-being, as thyroid hormones impact almost every cell and system in the body.
However, according to data published by the American Thyroid Association (ATA), thyroid diseases affect an estimated 20 million Americans, many of whom are unaware, leaving them at risk of potential serious long-term health consequences.1
Watch the video below to learn how to support optimal thyroid function.
5 common thyroid problems
Thyroid health is influenced by dietary and lifestyle habits, exposure to environmental pollutants, stress, genetic components, and hormonal shifts.
Due to this complexity, thyroid problems are widespread and often go undetected, making it essential to support thyroid health through balanced nutrition, stress management, and regular medical checkups.
Here are five common thyroid disorders and tips to promote thyroid balance naturally.
1. Hypothyroidism
Hypothyroidism is the most common thyroid condition. It occurs when the thyroid gland doesn’t produce enough thyroid hormone, slowing down many of the body’s functions.
“This type of thyroid disorder is often called underactive thyroid, and is most commonly caused by iodine deficiency, since iodine is an essential part of thyroid hormone structure and function,” explains Dr. Berg.
Other potential causes of hypothyroidism include autoimmune responses, pituitary gland dysfunction, and certain medications such as lithium and interferon-alpha.
Common symptoms of hypothyroidism include:
- Weight gain
- Cold sensitivity
- Unexplained fatigue
- Depression
- Constipation
- Sluggish digestion
- Dry skin
- Hair loss
- Brain fog
- Fertility issues
Obtaining adequate amounts of iodine through seaweed, iodized salt, fish, dairy, and eggs is essential for individuals with hypothyroidism, as iodine supports proper thyroid hormone production and overall thyroid function.
In addition, research published in Frontiers in Endocrinology highlights that the thyroid gland contains the highest concentrations of selenium in the body and that selenium deficiency is a major risk factor for many thyroid diseases.2
Selenium-rich foods such as Brazil nuts, sunflower seeds, fish, eggs, and mushrooms play a vital role in supporting thyroid hormone metabolism and are important components of a diet that promotes healthy thyroid function.
2. Hyperthyroidism
Hyperthyroidism occurs when the thyroid gland produces too much thyroid hormone, leading to faster metabolic processes and dysregulated cellular functions.
It’s also known as an overactive thyroid and is typically caused by autoimmune problems, thyroid nodules, or thyroid gland inflammation.
Symptoms of hyperthyroidism include:
- Difficulty gaining weight
- Rapid heartbeat
- Anxiety or irritability
- High blood pressure
- Frequent bowel movements
- Sleep problems
- Excessive sweating
Individuals with hyperthyroidism tend to benefit from avoiding high dietary intake of iodine to promote balanced thyroid hormone production and limiting caffeine to manage symptoms such as palpitations or anxiety.
In addition, it’s recommended that those with an overactive thyroid consume plenty of cruciferous vegetables such as broccoli, cabbage, kale, and Brussels sprouts.
These vegetables contain compounds called goitrogens, which can help naturally reduce thyroid hormone production by reducing iodine uptake in the thyroid gland.
Maintaining thyroid health depends on getting a variety of essential nutrients, making a health-focused and nutritious diet important for managing both hypo- and hyperthyroidism.
A nutrient-dense, low-carbohydrate diet such as Healthy Keto® can be especially beneficial as it emphasizes minimally processed whole foods while reducing gluten-containing foods, which may help support thyroid function.

3. Autoimmune thyroid disease
According to data published by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), autoimmune disorders are a common cause of both hypo- and hyperthyroidism.3
In cases of autoimmune disease, the immune system attacks the thyroid gland, causing inflammation and tissue damage, which disrupts its ability to produce hormones properly.
The two most well-known autoimmune thyroid disorders are Hashimoto’s disease, a leading cause of severe hypothyroidism, and Graves’ disease, the primary cause of hyperthyroidism.
While symptoms of Hashimoto’s and Graves’ disease mirror those of an underactive and overactive thyroid gland, they’re often accompanied by other autoimmune-related symptoms such as stiff joints, systemic inflammation, or skin problems.
In addition to making beneficial dietary changes in line with recommendations for hypo- or hyperthyroidism, those affected by an autoimmune thyroid disease often benefit from a gluten-free diet.
This has been confirmed by research published in Frontiers in Endocrinology, summarizing “Our results seem to indicate a positive effect of gluten deprivation on thyroid function and inflammation, particularly in patients with Hashimoto’s thyroiditis.”4
Gluten proteins are structurally similar to thyroid tissue, which may lead the immune system to mistakenly attack the thyroid gland through a process called molecular mimicry. This can worsen inflammation and trigger imbalanced immune activity, leading to impaired thyroid function and associated health issues.
4. Goiter
Goiter is another common thyroid disorder characterized by an enlarged thyroid gland that can be linked to thyroid hormone imbalance but may also develop in individuals with normal thyroid hormone concentrations.
Common causes of goiter include:
- Genetic predisposition
- Iodine deficiency
- Autoimmune thyroid disease
- Inflammation of the thyroid gland
- Thyroid nodules
- Hormonal changes
- Radiation exposure
Effective management of goiter depends on the exact underlying cause and highlights the importance of medical testing to evaluate an enlarged thyroid gland.
Increased dietary iodine intake may help in iodine-deficient individuals, while autoimmune-related goiters may benefit from nutritional strategies such as an anti-inflammatory diet and gluten avoidance to minimize immune system overactivity.
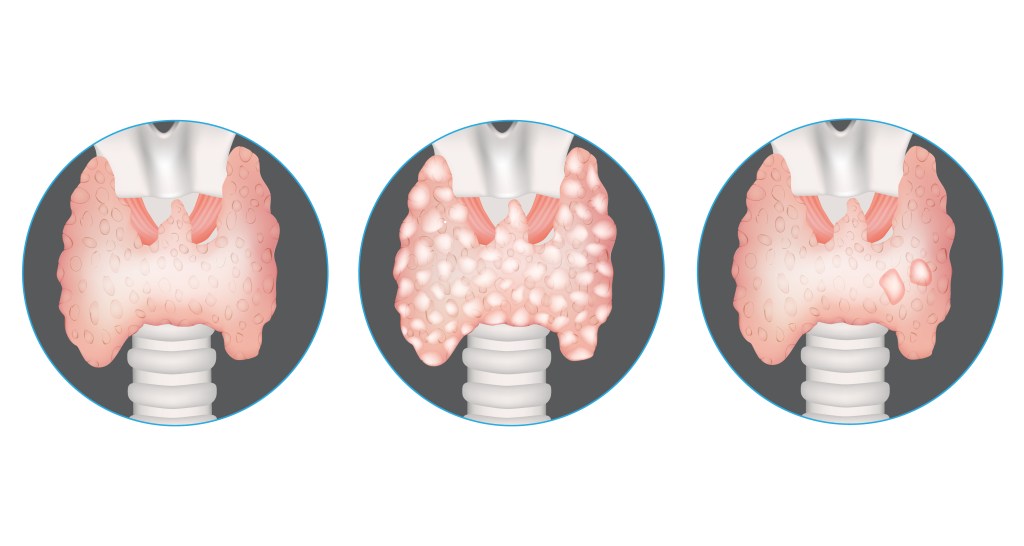
5. Thyroid nodules
Thyroid nodules are growths that form within the thyroid gland and are very common, especially in adults over 50.
Although most thyroid nodules are non-cancerous and don’t cause any symptoms, a small percentage may lead to hyperthyroidism or, in rare cases, may progress into thyroid cancer.
Consult a healthcare provider if you develop symptoms of thyroid nodules, such as:
- A lump or swelling in the neck
- Difficulty swallowing or breathing
- Hoarseness or voice changes
- Persistent throat discomfort
- Symptoms of hyperthyroidism
Similar to goiter, the management of thyroid nodules largely depends on the underlying cause and, in many cases, may not require pharmacological treatment or thyroid surgery, especially if the nodules are small, non-cancerous, and not causing symptoms.
However, individuals with thyroid nodules are advised to limit exposure to endocrine-disrupting chemicals, such as bisphenol-A (BPA) in plastics, phthalates found in many personal care products, and perfluorinated compounds commonly used in nonstick cookware.
These chemicals can interfere with hormone regulation and may negatively impact thyroid health. Reducing exposure can help support hormone balance and potentially reduce inflammation that can contribute to nodule development or growth.
When to talk to your doctor
If you have developed symptoms such as fatigue, unexplained weight changes, altered moods, cognitive problems, sensitivity to heat or cold, or changes in heart rate, it’s important to talk to your doctor about possible thyroid issues.
A doctor will likely order blood tests to check your thyroid hormone levels, which help determine whether your thyroid is underactive or overactive. In addition, imaging tests such as an ultrasound may be used to evaluate the size, structure, and activity of the thyroid gland.
In some cases, a radioactive iodine uptake test may be used to measure how well your thyroid absorbs iodine, an indicator of overall thyroid function.
You should also seek medical advice if you develop a lump in your neck, notice swelling, or experience difficulty swallowing or breathing, as this could indicate thyroid nodules or goiter.
In rare cases, the sudden onset of high fever, rapid heartbeat, confusion, or agitation may signal a thyroid storm. This is a potentially life-threatening complication of severe hyperthyroidism and requires immediate emergency care.
Key takeaways
- The thyroid is a butterfly-shaped gland in the neck that plays a key role in the body’s endocrine system.
- It produces the hormones T4 and T3, which regulate metabolism, temperature, and cellular activity under the control of the pituitary gland.
- Proper thyroid function is essential for overall health, but thyroid disorders affect millions of people, often without noticeable early symptoms.
FAQ
1. What are the most common thyroid problems?
2. What does the thyroid do?
3. What are the signs of a thyroid problem?
4. How does an underactive thyroid make you feel?
5. How do I support a healthy thyroid?
Sources
- General Information/Press Room | American Thyroid Association. American Thyroid Association. https://www.thyroid.org/media-main/press-room/ ↩︎
- Wang F, Li C, Li S, et al. Selenium and thyroid diseases. Frontiers in endocrinology. 2023;14:1133000. doi:10.3389/fendo.2023.1133000 https://pmc.ncbi.nlm.nih.gov/articles/PMC10080082/ ↩︎
- Thyroid Tests – NIDDK. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/diagnostic-tests/thyroid ↩︎
- Piticchio T, Frasca F, Malandrino P, et al. Effect of gluten-free diet on autoimmune thyroiditis progression in patients with no symptoms or histology of celiac disease: a meta-analysis. Frontiers in endocrinology. 2023;14:1200372. doi:10.3389/fendo.2023.1200372 https://pmc.ncbi.nlm.nih.gov/articles/PMC10405818/ ↩︎


















